In cardiology we have developed some amazing treatments, both procedures and medications that can improve patients wellbeing and also prolong their lives. However, as we all get older the risks of treatments and drug side effects increases and in our elderly patients it is more difficult to balance the benefits versus the risk of treatments.
An example of this is in the treatment of patients coming to hospital with heart attacks. For patients with a heart attack called a STEMI heart attack, where one of the blood vessels (coronary arteries) going to the heart is usually blocked by a blood clot, it is generally accepted that the best treatment for patients of any age, is to perform a coronary angiogram. This involves putting small plastic tube in either the arm or leg and then passing a long tube to the heart, through which dye can be injected. This allows us to visualise the blood vessels going to the heart. If a vessel is blocked then the same plastic tube can be used to pass a balloon into the blocked artery, which can then be inflated to open the vessel. This is called coronary angioplasty. A stent (a metal scaffolding) is often then expanded to keep the blood vessel open.
This treatment and other improvements such as medication changes have meant that the death rate of patients attending our hospitals with STEMI heart attacks has decreased from about 15% to 5% over the last 30 years. Patients are also less likely to have long term complications if they have had their artery opened. Although the complication rates in our elderly patients is higher, the benefits of this invasive treatment is also greater.
NSTEMI heart attacks are a bit different; they are the most common type of heart attacks and often occur when one of the blood vessels going to the heart has a blood clot in it but that clot does not completely block the artery. They can also be treated with angioplasty and stenting. We know from research studies that younger patients who present with this type of heart attack benefit from an angiogram. The findings from the angiogram then helps in decision-making about whether the patient is best treated with angioplasty and stent insertion, tablets, or coronary artery bypass surgery (CABG).
However, it isn’t known whether this approach is also beneficial in the over 80s. Up until now, these patients have often been treated with tablets only rather than being put forward for an angiogram because of concerns about the increased chance of complications from invasive treatments in older patients.
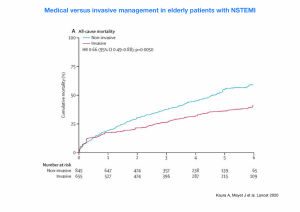
My research team at Imperial College London have recently found that patients presenting to hospital with an NSTEMI heart attack who were aged 80 and above and who weren’t very frail, had a death rate that was a third lower if they had a coronary angiogram compared with patients who were just treated with tablets. This indicates a very large benefit of invasive management in these older patients.
The red line indicates the death rate in patients who had an angiogram and the blue line shows the death rate of patients who didn’t. The death rate is about a third lower in patients who had an angiogram performed.
We published the findings in the Lancet and you can read the full research paper from the link below. The results, showed a large benefit for treating older patients in a similar way to younger ones. This study emphasises that the treatments that we offer shouldn’t be determined by biological age but rather should be based on how robust patients look and feel. It’s really important to discuss all options with patients of all ages so individuals can make a choice about which treatment is right for them.
Kaura A, Mayet J. et al. The Lancet 2020.
LINK: https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)30930-2/fulltext
Ageism in the NHS- does it still exist in 2024?