Why Choose Dr. Iqbal Malik at London Cardiovascular Clinic?
When making a health decision, choosing the right healthcare provider is essential. London Cardiovascular Clinic offers great care and coronary angioplasty expertise (PCI or PTCA). We are a top private healthcare provider in the UK.
Here’s why the London Cardiovascular Clinic is the top choice for a coronary angioplasty procedure in the UK:
- Recognised Expertise: Our highly skilled cardiologists, cardiac surgeons, and nurses specialise in coronary angioplasty procedures. Coordinated by Dr Iqbal Malik, a leading Consultant Cardiologist, our experts bring extensive experience and a patient-centred approach to ensure the best possible outcomes. Dr. Malik is a proctor for this procedure. He teaches and trains others and lectures on the topic worldwide, having 20 years of experience performing Coronary Angioplasty.
- Personalised Care: We understand that every patient is unique. Our dedicated team takes the time to thoroughly evaluate your condition and tailor the treatment plan to your individual needs. From the initial consultation to post-operative care, we’ll be with you every step of the way.
- Comfortable and Convenient Experience: Your well-being is our top priority. Our clinic provides a relaxed and welcoming environment, making your stay as pleasant as possible. We also offer flexible appointment times. We meet your needs to make the experience less stressful.
Do I Need PCI Surgery?
Deciding whether you need a coronary angioplasty procedure (PCI) involves consulting your doctor. They will consider many factors. These include your medical history, current symptoms, and individual risk factors for heart disease. PCI surgery might be recommended in cases of:
- Angina (chest pain caused by blockages) that doesn’t respond to medication.
- Reduced blood flow, causing symptoms like shortness of breath or fatigue.
- Severe narrowing or blockage in coronary arteries. These might NOT be causing symptoms but are so severe that they need to be tackled anyway.
- A heart attack (acute chest pain causing an Acute Myocardial Infarction (AMI)) due to blocked arteries. This is an Emergency.
The good news is that many blockages can be managed medically. However, some blockages are so severe that you may need Coronary Bypass Surgery (CABG) instead. Dr Malik will help you decide which is best.
Take a look at Dr. Malik. He is explaining the treatment options for coronary disease, including stenting (PCI):
What is PCI?
Percutaneous Coronary Intervention (PCI), also called coronary angioplasty, is a minimally invasive procedure. It opens narrowed or blocked coronary arteries. This helps blood vessels and improves blood flow to the heart, relieving symptoms such as chest pain and reducing the risk of heart attacks.
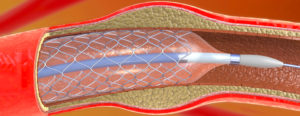
Below is a diagram of an artery during the coronary angioplasty procedure. There is a “stent” mounted on a balloon:
What Does Coronary Angioplasty Procedure Involve?
A coronary angioplasty procedure (PCI) requires local anaesthesia and involves the following steps:
- Preparation and Access: A small incision is made in the wrist (or groin) to access a blood vessel. A catheter (a thin, flexible tube) is inserted and guided to the coronary artery.
- Navigating the Artery: A very thin steel wire is navigated across the narrowing. Once the wire is positioned, a tiny balloon is slid over it.
- Inflating the Balloon: The balloon is inflated at the site of the narrowing to widen the artery. This cracks and stretches the plaque of cholesterol.
- Deploying the Stent: A stent (a small mesh tube) is often deployed to keep the artery open. In tougher cases, a rotablator ( basically a drill) may be used before deploying the stent.
- Completion: The catheter and other equipment are removed, and the incision site is closed, usually with a wristband to maintain pressure. Patients are usually kept overnight for monitoring.
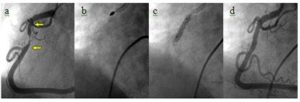
Below you can see step-by-step images of PCI where the narrowed artery (panel a) is opened up with a drill (panel b), then a balloon (panel c), and a stent inserted (panel d):
How to Prepare for PCI Surgery at London Cardiovascular Clinic?
Getting Here
Dr. Malik primarily sees patients at One Welbeck Heart Health, 1 Welbeck St, London W1G 0AR. Appointments at other locations can be arranged upon request.
Have questions or special needs? Make an enquiry today!
What Tests Will I Need Beforehand?
Before the procedure, you may undergo several tests, including:
- Electrocardiogram (ECG): Records your heart’s electrical activity.
- Echocardiogram: Ultrasound scan to create images of your heart.
- Blood Tests: Assess overall health and check for underlying conditions.
- Stress Test: to see if the narrowed artery is causing a problem
Note: It helps to bring a letter from your General Practitioner, prescriptions, old letters, and any previous CDs of tests (e.g., angiograms).
Treatment
After reviewing the test results, Dr. Malik will provide individual instructions on how to prepare for your PCI surgery. This may include dietary and/or medicinal adjustments.
Don’t hesitate to discuss any concerns or questions with the medical staff. They are dedicated to supporting you throughout your healthcare journey.
Book Your Consultation
Send us an e-mail or complete our simple contact form to arrange your consultation with London’s top cardiologist consultant, Dr. Iqbal Malik.
Coronary Angioplasty Procedure Recovery: What to Expect
Recovering from a coronary angioplasty is faster and easier than bypass surgery. Here’s what you can expect:
- Hospital Stay: Most patients can go home the same day or the day after the procedure. You will be monitored in the hospital for a few hours to ensure there are no immediate complications.
- Post-Procedure Care: You’ll receive detailed instructions on how to care for yourself at home. This includes wound care, medications, and activity restrictions.
- Medications: You will likely be prescribed blood thinners to prevent blood clots from forming around the stent. It’s crucial to take these medications as directed.
- Activity Restrictions: Avoid strenuous activities and heavy lifting for about a week. Light activities like walking are encouraged to promote circulation and healing.
Full recovery can take around a week. During this time, the stent will be fully integrated with your heart tissue. Follow all medical advice to ensure a smooth recovery.
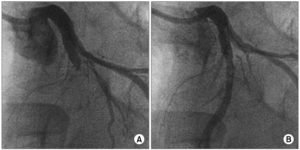
Below you can see a coronary angiogram before and after the coronary angioplasty procedure. This blood vessel was completely blocked in the middle of the picture and was opened up:
Frequently Asked Questions
What Are the Advantages and Disadvantages of Stents?
Advantages:
- Improved Blood Flow: Stents help open narrowed arteries, improving blood flow and reducing symptoms like chest pain and shortness of breath.
- Minimally Invasive: The procedure is less invasive than traditional open-heart surgery. It leads to a quicker recovery.
- Reduced Risk of Heart Attack: If you are having a heart attack, then PCI is lifesaving and abort it.
Note: If you have a narrowing, then the PCI is to help symptoms mainly. There are a few spots in the coronary artery tree, with large areas of the heart at risk, where PCI and stents MAY reduce the risk of heart attacks. However, this is rare, and stents are not used to “prevent” heart attacks. The tablets that you are given will do that, along with lifestyle changes.
Disadvantages:
- Risk of Re-Narrowing: In some cases, the artery may re-narrow after a stent is placed, requiring additional treatment.
- Blood Clots: There is a risk of blood clots forming on the stent, which is why blood thinners are prescribed.
- Procedure Risks: As with any procedure, there are risks, including bleeding, infection, and complications related to the catheter.
The risks of Angioplasty are much like those of Coronary Angiography. But, there are more specific risks of the Angioplasty procedure. These are usually damage to the coronary artery wall. They can provoke a heart rhythm issue or damage the blocked artery. This damage may require a bypass operation. This tends to occur in less than 1:200 patients treated.
To ease your mind, have a look at angioplasty in action by Dr. Malik:
How Much Does Angioplasty Cost in the UK?
Insurance
Most private medical insurance policies cover the cost of a coronary angioplasty procedure. To speed things up, contact your insurance company before your appointment. Get a pre-authorisation code. This will help you understand the specifics of what your policy covers and any potential out-of-pocket expenses.
Self-Funding
If you are self-funding your procedure, a detailed price list is available upon request and displayed in our waiting area. For a cost estimate, including the price of a private coronary angioplasty, contact our office. We can provide comprehensive information and answer any questions you may have about the financial aspects of your treatment.