Why Choose Dr. Iqbal Malik at London Cardiovascular Clinic?
When considering private ablation treatments for heart rhythm disorders, choosing the right specialist is important. We offer exceptional care and expertise for these types of ablations at London Cardiovascular Clinic, a leading private healthcare provider in the UK.
Here’s why London Cardiovascular Clinic stands out for private ablation procedures in the UK:
- Recognised Expertise: Dr. Iqbal Malik, a leading Consultant Cardiologist, specialises in assessing your condition holistically. If complex ablation procedures are needed, he will arrange it for you with one of his expert colleagues. Whether it’s AF ablation or catheter ablation for other things, Dr. Malik’s expertise ensures the highest quality care.
- Personalised Care: We understand that every patient is unique. Our dedicated team takes the time to thoroughly evaluate your condition and tailor the treatment plan to your individual needs. From the initial consultation to post-operative care, we’ll be with you every step of the way.
- Comfortable and Convenient Experience: Your well-being is our top priority. Our clinic provides a relaxed and welcoming environment, making your stay as pleasant as possible. We also offer flexible appointment times. We meet your needs to make the experience less stressful.
Do I Need Atrial Fibrillation or Catheter Ablation?
Private Atrial Fibrillation (AF) Ablation
According to the government’s Atrial Fibrillation NICE guidelines, ablation therapy is recommended for patients with persistent or symptomatic Atrial Fibrillation that doesn’t respond well to medication. While these guidelines are designed for public healthcare, private treatment options for AF ablation are also available in the UK. If you experience irregular heartbeats, shortness of breath, or fatigue, private AF ablation can target problematic heart tissue to restore normal heart rhythm and offer an alternative to public healthcare options.
Private Catheter Ablation
You might need catheter ablation if you have a heart arrhythmia that’s significantly affecting your quality of life or if other treatments haven’t worked. This procedure is a less invasive option, which helps you rely less on medication. While catheter ablation is available through public healthcare, you can also choose private treatment options in the UK for quicker service. It’s particularly effective for arrhythmias like atrial flutter or ventricular tachycardia, helping to keep your heart working normally. These ablations may be in the upper chamber Atrial), at the junction of the upper and lower chambers- AVNRT ablation or AV node ablation, or Ablation of an accessory pathway. Rarely, ablation is done on the lower chamber- VT ablation.
How to Prepare for Private AF Ablation and Catheter Ablation at London Cardiovascular Clinic?
Getting Here
Dr Malik primarily sees patients at One Welbeck Heart Health, 1 Welbeck St, London W1G 0AR. Appointments at other locations can be arranged upon request.
Have questions or special needs? Make an enquiry today!
What Tests Will I Need Beforehand?
Before undergoing any ablation procedure, specific diagnostic tests are essential to ensure the treatment is suitable and safe. Depending on the procedure, these tests help assess the condition of your heart.
Below is a list of common tests you may need:
- AF Ablation: Common tests for treatment for atrial fibrillation in the UK include an electrocardiogram (ECG) to monitor heart rhythm, an echocardiogram (TTE) to visualise the heart’s structure, and a Holter monitor to record heart activity over 24 hours.
- Other Catheter Ablation: Tests are similar to those for AF ablation but also most commonly Holter monitoring and frequently a functional Exercise test. In addition, an MRI scan may be needed to assess the structure of the heart in more detail.
These tests provide necessary information for Dr. Iqbal Malik about your heart.
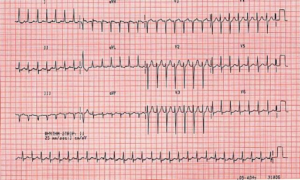
Below is an example of an ECG of a fast heartbeat (AVNRT) that can be cured by ablation:
Treatment
After reviewing the test results, Dr. Malik will provide individual instructions on how to prepare for your chosen ablation. This may include dietary and/or medicinal adjustments.
Don’t hesitate to discuss any concerns or questions with the medical staff. They are dedicated to supporting you throughout your healthcare journey.
What Happens During an Atrial Fibrillation or Catheter Ablation?
Here’s a clear step-by-step guide to what happens during the chosen ablation procedure:
During Private AF Ablation:
- You will receive a combination of local anaesthetic and sedation to ensure comfort throughout the procedure. The procedure is often done under general anaesthetic (GA) to increase comfort.
- A Transoesophageal Echocardiogram (TOE) is performed to confirm there are no clots in your heart.
- A catheter is inserted into a vein in the groin and guided to the heart using X-ray fluoroscopic guidance.
- The catheter is advanced to the right side of the heart, and a needle is used to enter the left atrium, where radiofrequency energy is applied to target spots and destroy abnormal tissue causing atrial fibrillation.
- Post-procedure, you will be monitored in a recovery area for a few hours to check for immediate complications and follow-up visits will be scheduled to assess the procedure’s effectiveness.
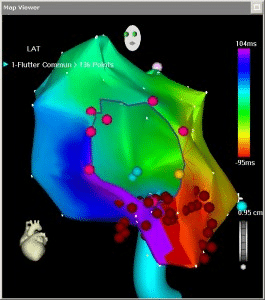
Below is a “map” of the left atrium generated during ablation:
During Private Catheter Ablation:
- Local anaesthetic and sedation are administered to keep you comfortable during the procedure. Again, GA may be used
- A catheter is inserted into a vein, usually in the groin, and guided to the heart with the help of X-ray fluoroscopic guidance.
- An Electrophysiology (EP) Study is conducted to identify the exact areas of the heart causing abnormal rhythms.
- Radiofrequency energy or cryoablation is applied to the identified areas to disrupt the abnormal electrical signals.
- After the procedure, you will be observed for a short time to monitor for any complications, and follow-up appointments will be scheduled to evaluate the procedure’s success and adjust treatments as necessary.
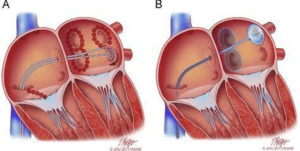
Diagram of Catheters crossing from the right atrium to left atrium to perform ablation.
Book Your Consultation
Send us an email or complete our simple contact form to arrange your consultation with London’s top cardiologist consultant, Dr Iqbal Malik.
AF Ablation and Catheter Ablation Recovery: What to Expect
Recovering from ablations is generally straightforward. Here’s what you should expect during your recovery:
Recovery After AF Ablation:
Recovery from AF ablation generally proceeds smoothly. After the procedure, you’ll be monitored in a recovery area for a few hours. Most patients can return home either the same day or the next day. You should avoid strenuous activities for at least a week and focus on light activities, such as walking, to aid in your recovery. Some chest discomfort or irregular heartbeat may occur initially, but these symptoms usually resolve as your heart heals. Regular follow-up visits will be scheduled to ensure the procedure is successful and to adjust any medications if needed.
Recovery After Catheter Ablation:
For catheter ablation, you may require a short hospital stay. Typically, you will need to rest for a few days and can gradually resume normal activities within a week. It’s common to experience minor bruising or swelling at the catheter insertion site. Follow-up appointments are crucial to monitor your heart rhythm and assess the long-term success of the procedure. During the initial recovery period, avoid heavy lifting and intense exercise as advised by your healthcare provider.
Regular follow-up visits are essential to monitor your heart health and the effectiveness of the ablation procedure.
How Much Does Private Atrial Fibrillation or Catheter Ablation Cost in the UK?
Insurance
Most private medical insurance policies cover the cost of ablations. To speed things up, contact your insurance company before your appointment. Get a pre-authorisation code. This will help you understand the specifics of what your policy covers and any potential out-of-pocket expenses.
Self-Funding
If you are self-funding your procedure, a detailed price list is available upon request and displayed in our waiting area. For a cost estimate, including the price of a private AF Ablation and Catheter Ablation, contact our office. We can provide complete information and answer any questions you may have about the financial aspects of your treatment.
Frequently Asked Questions
What Are the Risks of Ablation?
While any type of ablation is generally safe, there are some risks to consider:
- AF Ablation Risks: The risks associated with AF ablation include bleeding, infection, and, in rare cases, damage to the heart or blood vessels. There’s also a small risk of stroke during the procedure. Most complications are minor and can be effectively managed with prompt medical care.
- Catheter Ablation Risks: Catheter ablation risks are similar to those of AF ablation, with potential complications including bleeding, infection, or damage to the heart’s electrical system. There’s also a chance of a recurrence of the arrhythmia, which might require further treatment.
Bruising at the insertion site is common but typically resolves on its own.
Your doctor will review these risks with you before the procedure and answer any questions you may have.
What Are the Benefits of Ablation?
AF Ablation Benefits
The primary benefit of AF ablation is the potential to restore normal heart rhythm, reducing or eliminating the symptoms of AF. Successful ablation can improve your quality of life, decrease the need for medications, and lower the risk of stroke.
Catheter Ablation Benefits
Catheter ablation offers the possibility of curing arrhythmias without the need for long-term medication. Many patients experience significant improvements in symptoms and a reduced risk of arrhythmia-related complications.