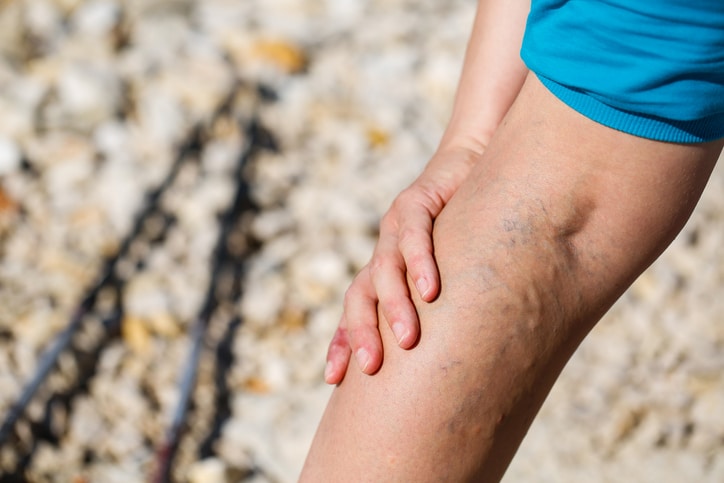
Varicose veins are so common, that it is difficult to avoid knowing something about them. You may be aware of prominent veins on your own legs, or have noticed that a family member or friend has obvious clusters of swollen and winding ‘snake-like’ veins, or developed more subtle skin markings from the small veins within their skin. Either can be a sign of an underlying problem with your veins.
Any medical dictionary will tell you that varicose veins are “dilated, tortuous, elongated, superficial veins with non-functioning, incompetent valves.” Instead of blood returning promptly to the main veins and back to the heart, leaky valves can cause blood to pool in the leg veins, increasing the back pressure in the venous system, and causing the veins to swell, ache and leak fluid and blood into the leg tissue. This sets up a process of inflammation, and changes to the microcirculation ensue, which effect oxygen and nutrient delivery to the tissues.
What was only recently appreciated, however, from large population studies performed in Edinburgh, the US and Germany, is that as many as 2 out of every 5 people in the entire population have varicose veins. What is more, varicose veins are as common in men as they are in women.
Varicose veins may be visible just by looking at the leg, on clinical examination, or become apparent using ‘hand held doppler’ scanning, or ‘ultrasound imaging’ to examine the veins in detail.
What are the consequences of having varicose veins?
Varicose veins cause significant and often debilitating symptoms, ranging from throbbing and aching pains, itching and leg swelling, all of which may be worse in the evening, after prolonged sitting or standing, to unsightly skin changes and discoloration, hardening of the skin and underlying tissue, eczema, blockage of the surface veins (thrombophlebitis) which may rarely progress to the deep veins (causing DVT), ulceration and bleeding.
Should I seek treatment?
While many people still do not seek timely medical help for their symptoms, the treatment of varicose veins has advanced in leaps and bounds over the last ten years, and the published evidence clearly shows the benefits of medical, and particularly appropriately selected modern surgical treatment, in terms of symptom relief of and improved life quality.
Recently published 2013 NICE guidelines have consequently rejected the idea of delaying varicose vein treatment until signs of advanced disease are present, preferring instead to adopt a preventative approach and treat all patients with symptomatic varicose vein reflux.
This reflects the fact that varicose veins, when left without adequate treatment, ultimately progress to the point where their effects are harder or impossible to reverse (eczema, thrombophlebitis, discoloration and pigmentation, marked ankle swelling and venous ulceration).
People who develop varicose veins do so primarily due to a genetic tendency, and may need several treatments in the course of their life. This is not necessarily a failure of treatment, but reflects the natural history of varicose vein development.
Click here to see Mr Jaffer explaining how modern varicose veins surgery is performed as day case surgery. The various treatment options for endogenous vein ablation are discussed as well as pros and cons of differing strategies.
How can I be sure of getting the best treatment?
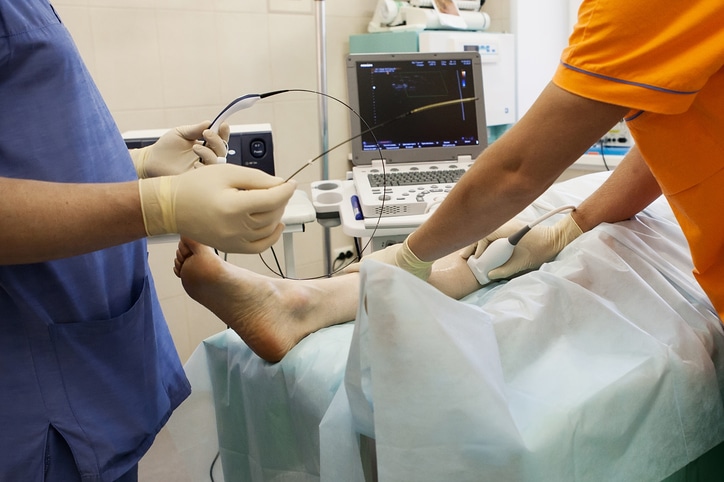
The first step is accurate assessment and diagnosis. Mr Usman Jaffer, our expert clinician, will speak to you to find out about your symptoms and concerns, your past medical problems and general health and whether you’ve had any previous surgery or treatment for your veins or another condition. We will then assess your veins with a hand held Doppler scan, performed in the clinic, and our expert vascular scientist will perform a comprehensive scan of your deep and surface veins as part of your initial ‘one-stop’ consultation.
In this way we will be able to assess the health and physiological function of your deep and surface veins. It is not safe to offer you advice or treatment without performing this full check-up, as it can lead to incorrect, partial or sub-optimal advice and treatment, which could potentially fail, or even make your condition worse.
One treatment for varicose veins is to use radiofrequency/laser ablation. If your veins can be treated by this minimally invasive technique, then after preparing the leg in a sterile manner, your surgeon will use ultrasound to identify the main surface veins that need treatment. A little local anaesthetic is injected at the point of entry to the vein, and a needle is used to insert the treatment catheter into the vein. Once this treatment device is properly positioned, a dilute local anesthetic solution is injected around the target vein using ultrasound. This ‘tumescent anaesthesia’ makes the heat treatment process itself painless, but involves a series of small injections along the vein before the heating begins. Most people tolerate this procedure well without a general anaesthetic, but if you need to have a large number of vein avulsions in addition, you may be best served by having it performed under general anaesthetic.